What Battling Covid-19 is Really Like: Local ER Doctors Speak Out
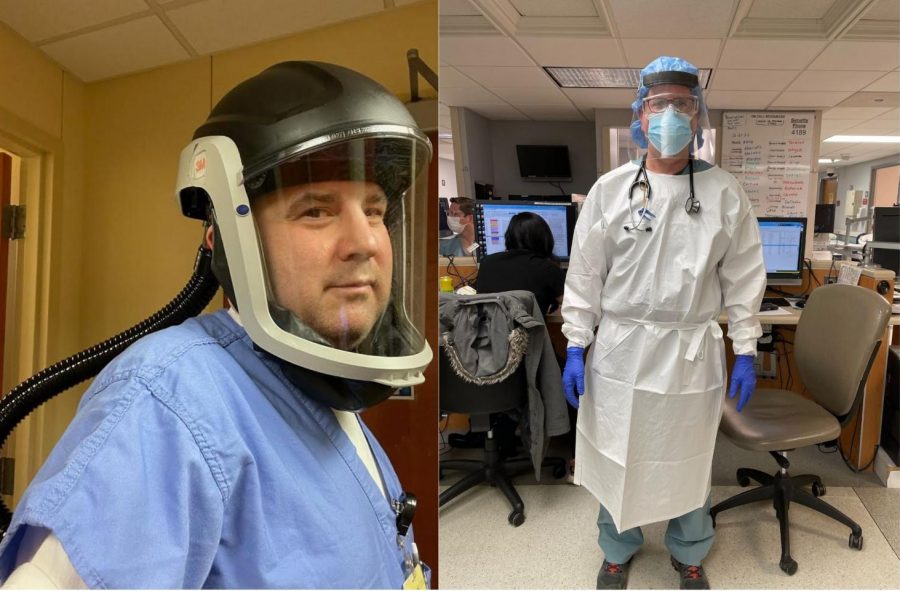
The staff in AMITA Health Resurrection Medical Center Chicago and Advocate Good Shepherd Hospital, including Dr. Sharp (right) and Dr. Greenberg (left), are making sure to take every precaution, such as rubber gloves, face masks and shields, eye protection, and more, to keep themselves safe.
Millions of frontline health care workers across the United States have been battling Covid-19 for nearly a year and have faced many challenges regarding high patient volumes, the risk of infection and the emotional strain as cases continue to rise daily. In Libertyville and the surrounding suburbs, as well as in Chicago, many emergency physicians have been treating Covid-19 patients during their daily battle against the virus.
Dr. Halleh Akbarnia has two children who attend LHS and is an emergency physician at Advocate Condell Medical Center in Libertyville. She has been treating Covid-19 patients since the start of the pandemic. In the early stages of the virus back in March and April 2020, Dr. Akbarnia recalls how treating Covid-19 was like “dealing with something you can’t see and something you don’t really know.”
At the time, nobody knew how many people Covid-19 would infect and kill, along with how many people would show symptoms and side effects, according to a report released by the Centers for Disease Control and Prevention last March.
“That was the part that was the most anxiety provoking for me,” said Dr. Akbarnia. “Just not knowing what we were dealing with. I wasn’t even as worried for myself; I was more worried about what I could do or bring home to my family.”
As a frontline health care worker, she said she has to mentally prepare herself for every shift, each of which generally ranges from eight to 10 hours long.
“I would go to work and sit outside in my car, and I think probably for the first time in my life, I experienced what anxiety felt like,” she said. “I felt panic out there [and I remember] thinking, ‘I just need to breathe before I go in, just like you’re going into the biggest game of your life.’”
Additionally, Dr. Akbarnia worries that her high exposure to Covid-19 will bring the virus home to her family. After her shift, she takes off her hospital gear in her garage and takes a shower before hugging her kids. “You always have [the thought of infecting your family] in the back of your mind,” she said.
Emergency physician Dr. Jay Sharp works at AMITA Health Resurrection Medical Center Chicago and has also been treating Covid-19 patients since the beginning of the pandemic.
“It really hasn’t been like anything I’ve ever experienced before as a physician,” he said. “It’s a totally different disease from what we have ever seen, and it took us by surprise by how sick people were.”
Although hundreds of thousands of new cases of Covid-19 are still being diagnosed every day throughout the country, Dr. Sharp said that over that past 10 months, he has found that “people who are getting [Covid-19] aren’t as sick as they were earlier in the pandemic, and I think that goes along with some of the reports and some of the medical studies that I’ve read.”
Dr. Sharp added that, similar to the 1918 influenza pandemic and general trends of past viruses, the disease has mutated into a more infectious but less deadly strain and “seems to fit into what I’ve been experiencing personally.”
Early on in the pandemic, patients coming into the emergency room were so sick that Dr. Sharp and his team tried to “batch” all of their procedures, essentially completing all of their treatments at once. Depending on how ill the patient was, the doctors would determine if they needed to be put on a ventilator or needed intubation. “We would spend maybe an hour, an hour and a half in a room with a patient trying to get everything done [that] we needed to do, so that we could not waste the PPE,” he explained.
Dr. Sharp uses a wide variety of personal protective equipment (PPE) to minimize his exposure to Covid-19 patients in the emergency room: a N95 respirator mask, and an additional surgical mask layered on top of that, along with a head covering, cap, face shield, gown and two pairs of gloves.
While PPE gear is highly effective, Dr. Sharp and his colleagues try to put Covid-19 patients in negative pressure rooms, isolated hospital rooms where the contaminated air is sucked outside, but with the surge of infections after the holidays, his team resorted to seeing patients in all available spaces.
Dr. Manish Acharya, whose son is an editor for Drops of Ink, is also an emergency physician, but his job mainly focuses on administering and staffing hospitals in Illinois and Wisconsin as well as overseeing the telemedicine services for the hospital. At the beginning of the pandemic, “the greatest challenge was understanding the disease and understanding how it spread and getting a comfort level of that,” he recalled.
Now that health care workers have a better understanding of Covid-19, Dr. Acharya’s challenges have shifted to taking care of an emergency department: “We used to be able to admit a patient and they would be able to go to the ICU, but now we’re finding that we may need to transfer a patient two to three hours away because all ICUs are full.”

(Jake Short )
Similarly, Condell Hospital has been experiencing an overflow of Covid-19 patients. The hospital is set up to handle a certain number of patients, said Dr. Akbarnia. “We have maximized that [space]; every day our ICUs are full,” she said. “Even when people say, ‘Oh, there’s still 20% space’ or ‘Our hospitals are doing better,’ [the hospital is] doing better, but ICUs as we know them before [the pandemic] are always 100% full.”
Medical professionals have turned to creating new ICU space on other floors of the hospital, continuously increasing ICU space.
Dr. David Greenberg works for Tri County Emergency Physicians, which staffs the Advocate Good Shepherd Hospital in Barrington. He does not represent and is not an employee of Advocate Health Care.
Dr. Greenberg suggests the recent rise of Covid-19 cases in early January is due to new strains of the virus making it more easy to be transmitted from one person to another. “Other reasons why [cases] are going up are recent holidays, Thanksgiving, Christmas and New Year’s, so as more people are together in a closed space, especially if they’re not following true social distancing [and] wearing masks, there’s more opportunity for the virus to spread,” said Dr. Greenberg.
Dr. Akbarnia expressed how she thought that a lot of these infections and deaths during the holidays were preventable. “The second [wave of infections], I was much more frustrated because I knew a lot of [infections and deaths] should have not happened,” she said.
Condell Hospital never experienced a shortage of PPE in the early stages and later months of the pandemic. Dr. Akbarnia explained how in the spring of 2020, the surrounding community was able to donate masks and medical supplies to the hospital, so frontline workers always had a backup in case supplies ran out.
Dr. Akbarnia has also worked at Chicago hospitals during the pandemic and recalled how “some of my colleagues would have to sometimes use one mask for four days until they were able to use another one, never knowing if it was actually protecting them.”
At Good Shepherd Hospital, Dr. Greenberg said that last spring, “we were never without [supplies], but there was certainly control over the supply.”
Another difficulty that health care workers are facing is the struggle of patients who come into the hospital without their loved one. “It is a huge challenge not to be able to handle both the patients that are in the hospital but also to have to communicate what’s going on to the families who are at home or just sitting by the phone waiting for any information,” explained Dr. Akbarnia.
However, new remote technology and practices have drastically changed the way doctors communicate, whether it’s diagnosing a patient or keeping family updated.
Telemedicine is an online health care service that allows physicians to communicate with patients remotely. “[It decreases] some of the stressors on patients as well as physicians by limiting their exposure [to Covid-19] by direct contact,” explained Dr. Acharya. He added that the service is transforming health care systems because more doctors are consulting patients virtually because they are required to keep them out of doctors’ offices.
All four medical physicians mentioned above have received both doses of the Covid-19 vaccine. Said Dr. Akbarnia, “It’s a relief, and I just feel like I can’t wait for everyone else to get this protection as well.”
Dr. Akbarnia is now working with the city of Chicago and surrounding counties to try to get more volunteers to help vaccinate people. However, a recent shortage in vaccines has halted her efforts, frustrating many in the community and herself. Furthermore, there isn’t a very good system in place yet for high-risk senior citizens to sign up for vaccines via the Internet because “not all of them use electronics.”
“I think the public is very tired of Covid and people are tired of restrictions, but they really do make an impact on the ability to limit the spread of the virus,” said Dr. Greenberg. “I think as long as people are practicing social distancing and wearing masks, we can hopefully begin to reopen in a more controlled fashion and get close to normal.”